The Gwent Mental Health and Learning Disability Partnership Board
International Mental Health Collaborating Network
Whole Life-Whole System for People in Crisis
Acute and Crisis Development
1. Introduction
The current service model for acute and crisis services in the UK is under great pressure with high levels of demand and inappropriate referrals. The acute in-patient services are reporting 100% occupancy rates. In some places there are issues with the availability of Mental Health Professionals. This is the case in all Health Boards in Wales including ABUHB.
The current services are not sustainable and in many ways not meeting the whole life needs of service users.
There is a need for radical new thinking to how Acute and Crisis services are provided for individuals with their unique needs.
Several reports (Mind, Schizophrenia Commission,Crisis Concordant, etc.) have highlighted the need for services to be transformed into better ways of helping people when they are in need of crisis services and support.
Service users in the Wales National User Forum have been saying that,
- “Five minutes will be woefully inadequate to convey the views of the service users and carers who have needed the help of crisis intervention services and found these services lacking”
- “Service user and carer engagement needs to inform service provision and not vice versa”
- “Service user and carer 'involvement' must be about genuine and respectful dialogue and influence via input into the formation, development and evaluation of all service”.
A Gwent Whole Life-Whole System, Recovery Action Learning Set was established and
co-facilitated by ABUHB and the IMHCN.It was decided during the Learning set to focus on the Acute and Crisis Services to improve the experience of users and family members.
In the Gwent Action Learning Sets we have identified the issues that need addressing if we are to better meet the needs of users and family members as well as reducing the pressure and burden on staff that work in the acute and crisis services.
The current services have been working well but they are under pressure, as they do not have any alternatives for people in crisis other than the in-patient beds. They also have a number of inappropriate referrals whose unique needs could better be met by other complementary and alternative services.
The Action Learning Sets members, service users, family members, health professionals, managers, community organisations, police, ambulance services, A&E consultant have worked collectively to produce this Gwent Whole Life-Whole System : Acute and Crisis Service Model.
2. Current Service Issues
Health Service
The Gwent services for people in Crisis were designed several years ago. They are based on the model of services that consist of an acute in-patient ward or unit with a Crisis Team. This was developed as part of the UK wide Good Practice Policy Implementation Guidelines in 2005 in Wales.Many of the aspirations of this have been met but others have not. See, Welsh CRHT PIG.pdf
Since this time there has been a significant change in the profile, characteristics and needs of people seeking help in a crisis.
There are more people with complex needs, their social circumstances are very difficult,
more people are being subject to sectioning under the Mental Health Act.
3. The Need to Change and Develop
The need to improve the experience for people in crisis was identified by each member of the Learning Set. All participants were agreed that the present system was not working and not sustainable.
The following comments were from the workshop that was held in the Learning Set,
Feedback from people who use the service
- People not getting the service they feel they need
- Services are focussed around sets of criteria; rather than individual needs
- People are unable to access the service easily, especially due to multiple service lawyers, hoops and barriers
- Care dictated by the present system rather than what matters to the person
- Too much duplication in assessments in system
- Inconsistent relationships with staff in different parts of the service
- Not feeling that there’s time to be heard
Feedback from people who provide the service
- Staff feeling overwhelmed with the workload
- Staff not able to focus on the work they feel is valuable
- Staff are under pressure to “meet targets”
- Too many teams: too many interfaces: the Individual has to move through several teams
- Too many barriers between teams: relieve the system and improve capacity so that we can do things differently
- Some people have fixed belief systems in people, need to change and reflect on their practices
- Difficult to recruit staff in some areas (For example Middle Grade Doctors, AMHP’s, OAMH Inpatient Nurses)
- Staff overwhelmed with workload: spending more time with paperwork than engaging with users and families
- Acute wards: there is not much therapeutic interaction due to the pressure of work and user needs
- ‘Floater staff”: go around when the other staff are busy and provide a listening service
Gwent User and Carer Stories
“I came into secondary services, having been referred via family services in Llyn Onn – I was kept waiting for a very long time for an assessment. I was very lucky that Ewa kept me in family services during the wait (some 8 months), she was worried about me and wanted to keep an eye on me. I then had my assessment, but this didn’t mean that I was going straight into secondary support – I was kept waiting yet again. In limbo, but still having Ewa’s support – she was amazing. I think it was about 14 months from original referral until I was seen by the Clinical Psychologist in secondary services. There was no support in place to help me during this waiting game – but luckily Ewa was there” ( Extract from story. full text attached)
Staff Story
“I was on-call Saturday. I received a telephone call from Talygarn ward at 6:10am informing me a patient had arrived for assessment. When I arrived I discovered that the patient, a lady aged 72, had in fact presented to the Royal Gwent hospital in Newport at approx. 8pm Saturday night after an overdose.
She had been assessed by A&E as medically fit and was referred to psychiatry at approx. midnight at which point ambulance transport was booked to transport her from Newport to Pontypool
Ambulances were busy and this did not happen until 6am.
My lady was accompanied by her elderly husband of 78yrs. Both were made to sit in A&E from the time of arrival until the ambulance transport came, no bed or refreshments were apparently offered.
My lady was understandably exhausted when she arrived to me, having had no sleep at all.
I felt ashamed that we could treat people in such a manner and I felt guilty that despite the fact I knew she was exhausted I now had to ask her many more questions and perform a comprehensive risk assessment.
On my drive home I reflected upon what kinds of answers I may have given to my questions had I been sleep deprived on top of my already acutely distressing situation that had caused me to overdose”
4. Supporting Statistics
The following statistics gives an indication of the demand and pressure on the current services that makes the present system not sustainable.
This could include, for each locality in Gwent,
- No. of admissions to the acute ward/unit
- No. of re-admissions to the acute ward
- No. of referrals to the Crisis Team from, A&E, Police, GP’s, CMHT’s,
- No. of inappropriate referrals to the Crisis Team.
- No.of people taken on by the Crisis Team and those that referred to other services
- No. on the case load of CMHT’s and Crisis Teams
- No. of people waiting, in need of Housing
- Average length of stay in the acute ward
5. The Local and National Context
It has long been recognised across the country that people in crisis and in need of personal services are not getting a prompt response, finding it difficult to get access, being passed from one service to another with many barriers and their whole life needs are not properly addressed.
Furthermore the service has not enough choices available and very often people are admitted when their needs can be better met if there were alternatives available in the community.
Several national reports have time and time again identified the problems in the present service model and have made recommendations of what needs to be done to improve the experience for service users and their families. Yet very little has changed in recent years. There have been excellent exceptions to this in places like Bradford, Hertfordshire.Leeds
In Wales other Health Boards, Hywel Dda, ABMU are also addressing the problem. and developing new ways of thinking and working.
The Crisis Concordant is being developed in Wales and Gwent and this will make a valuable contribution when the plans are implemented.
Th Gwent Whole Life-Whole System: Acute and Crisis Model and Plan is fully compatible with and complementary to the Crisis Concordant.
An important part of the Learning set was knowledge about innovative services in the UK and other countries.
This was done through study visits to Trieste, Bradford and Hertfordshire.
A Twinning Collaboration with Trieste will be organised and facilitated by the IMHCN.
Wales National User Forum
This was established as a part of the National Partnership Board.
It has campaigned for improved mental health services, particularly for people in need of improved crisis services.
Mind Report, “Listening to Experience, An independent Inquiry into Acute and Crisis care”
“Crisis houses have often been set up in direct response to demand from mental health service users as a preferred alternative to hospital treatment (Faulkner, 2002). However, non- hospital crisis services do not necessarily have to be residential.
A series of research articles published in a British Journal of Psychiatry supplement showed greater service user satisfaction in residential ‘alternatives’ than with inpatient care. Service user experiences of alternative, non- hospital services appeared to be more positive overall, with reports of this type of care offering minimal coercion, maximum freedom and autonomy, safety and opportunities for peer support (Gilburt et al., 2010). Service users also reported less anger and aggression in alternative services (Osborn et al., 2010)”
Schizophrenia Commission, “The Abandoned Illness”
“One hundred years after the term “schizophrenia” was coined to describe severe psychosis, the Schizophrenia Commission came together to examine the provision of care for people living with psychotic illness. We are an independent group which took evidence from around the country and heard from several thousand people over 12 months. What we found was a broken and demoralised system that does not deliver the quality of treatment that is needed for people to recover. This is clearly unacceptable in England in the 21st century”
Crisis Concordant
The UK Crisis Concordant was introduced in response to the inappropriate placement of service users in police cells.
A Gwent Crisis Concordant is being developed which includes,
6. Whole Life-Whole System Vision and Model
The Vision for a Whole LIfe - Whole System Approach to meet the unique needs of people in Crisis is based on the following values and principles.
Furthermore the Approach and Model is designed to recognise the social determinants of mental health and addressing these relating to the individual’s needs.
The practice in all parts of the Whole System should be based on Recovery and Discovery principles; trusting and reciprocal relationships, shared responsibility, nothing about me without me, a trialogue approach.
Values
These were developed and agreed by all members of the Learning Set
- We will treat you as an individual and respond to you when you need us.
- We will treat you with dignity, compassion, empathy, respect and kindness at all times.
- We will treat you as an individual.
- We will work together with you and people who are important to you.
- We will be open and honest.
- We will strive to support you to keep yourself safe and act in your best interests.
- We will not decide anything for you or do anything to you without talking to you.
Principles
The key principles in defining a whole systems, recovery approach to respond to a critical time in a person’s life (before or during a crisis) are:
- Recognition of a dramatic emotional or circumstantial upheaval in a person’s life that should lead to recovery and not a path of deterioration.
- A critical time for reflection and positive growth, self determination – not a time for continuing pathways of hopelessness and /or maintenance.
- A time for change for the person to look at their life as a whole not just their mental health problem.
- The causes of a crisis need different solutions from various sources, financial difficulties, physical health, work stress, environmental factors, family problems etc.
- The contact and relationship formed between the user and professional in one part of the service should be the same trusting therapeutic relationship in all parts of the service system.
- The importance of shared responsibility between the user, family member, professionals and the organisation to create positive risk taking.
- Our hypothesis is that Whole Life, Recovery acute and crisis community services must be conceived as alternatives to a fixed place and to the conception of treating illness that is based on reductionist psychiatry, which contain and impoverish the individual's experience as a whole person.
- Services should be not only be tailored on illness management or social behavioural problems, but around the person and his/ her personal history and experiences.
- Making full “use” of the person’s crisis to move forward.
- Crisis is about resolution through multiplying community resources.
- Crisis is increasing information and knowledge around the person’s whole life needs.
- Crisis is increasing communication within the service and community as a social visibility.
Thus the need for a strategic and effective approach that is unique and humane with a comprehensive and open new viewpoint.
These values and principles are difficult to realise if there is an incomplete whole life - whole system service design and approach.
System thinking are a discipline for seeing wholes not holes. Its essential framework is developing interdependence and interrelationships rather than static and separate parts.
The common purpose of the whole should promote and embrace all the values and principles and the parts of the system must be sensitive to their contribution in achieving the overall purpose.
They should actively promote recovery, self-determination and growth for the individual by benefiting from both the mental health whole systems service and a community’s natural resources.
The Whole Life-Whole System : Acute and Crisis Model (see illustration below) includes the components outlined below. but could include other good practice models from the UK and other countries.
These can be implemented in an incremental way over the next 5 years to assess their effectiveness in meeting the needs of service users and in determining the number and place of in-patient beds required for Gwent.
The health and social services cannot and should not do this on their own.
This will require building partnerships with community organisations and groups who can provide some of the services.
The Gwent Whole Life-Whole System Service Model
The Gwent Learning Set looked at good practice in Acute and Crisis services that have been developed in the UK and other countries. Some of these were examined to see if they were appropriate to meet the circumstances and needs in Gwent.
We then put these together to form the following Gwent Whole Life-Whole System : Acute and Crisis Model.
A Users Pathway
At present people with mental health issues access the services through the following routes,
- A&E Liaison Service
- Police (Section 136)
- CMHT’s
- Crisis Teams
- GP’s
ABUHB has been working to simplify and improve the way in which people can have one access point to the services. The model is being developed incrementally; A Triage Service would take ownership of the referral to ensure that people are not bounced from one part of the service to another and by employing a mental health triage tool to ensure that the person receives an appropriate assessment by the correct part of the service in a timely mannerThis would need to enable service users to have open access so that prompt help can be given to the person when in crisis.
The pathway for users and family members through the service should be smooth with no barriers in place.
This is shown in the diagram below
The current services are in green font and the developing ones in blue font.
Acute and Crisis Service Pathway
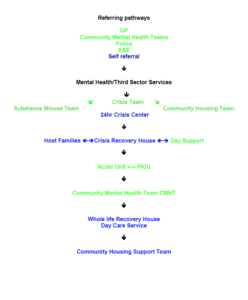
The Components of the Gwent Service Model
These will build on and complement the present Acute and Crisis services in each locality in Gwent.
Acute in-patient unit
Crisis Team
24 hr Single point of Access with self referral
“When I need urgent help to avert a crisis I, and people close to me, know who to contact at any time, 24 hours a day, seven days a week. People take me seriously and trust my judgement when I say I am close to crisis, and I get fast access to people who help me get better”( Crisis Concordant)
This needs to be made available in every Locality in Gwent.
Mental Health Support, First Responders
A&E Rapid Assessment, Interface and Discharge (RAID)
The RAID service developed in Birmingham represents an evolution of the liaison model and an approach, which undoubtedly improves the quality of care for people with mental ill health in an acute hospital. The economic analysis, however, shows that at the same time such an approach has the potential to save very significant amounts of money for the local health economy. As such, these services should be of particular interest to all those who provide acute hospital and mental health services and this should be especially true also for commissioners.
Host Families (Hertfordshire Trust and Liile, France)
These are based on the experience of adult fostering schemes but take this forward to provide a family support and natural home environment structure for individuals during their acute crisis. The Crisis Team team supports the host family. It is a short-term placement for up to 3 weeks. The host families are recruited, given training, and paid. Sometimes they are also used to place people to prevent a relapse and early discharge.
Users record a very positive experience from these and they are highly valued by the host family and mental health professionals. In some places they have greatly reduced the use of acute in-patient beds. They are a very cost effective alternative to expensive in -patient beds.
Pre-Crisis Sanctuary Houses (Leeds and Hertfordshire)
Different models of this service have emerged over the last 10 years in the UK and Internationally.
These have been developed as a more homely, small scale place of sanctuary. Some are not residential but there are advantages by having guest beds available. They provide the time and space for the user to reflect on their life history, to use their life story and strengths to counteract the episode in their life that is causing their distress or crisis. In some places these have been provided for specific groups, women, minority ethnic groups, etc.
These are also referred to as peer – run crisis houses.
They have a strong recovery and natural self help ethos.
They are sometimes managed and run mainly by service users.
They provide many alternative coping strategies, opportunities for self determination, massage, counselling, skills training, meditation, faith, art and culture, sport and leisure, reinforcing responsibility etc.
They reach out to encompass the natural resources of a community to help the user with their social issues.
They are usually managed by the 3rd Sector with Health and Social Services support.
Crisis Houses as alternatives to Acute In-Patient Units (Cardiff)
Crisis houses are a short-term residential alternative to acute in-patient stay for people in mental health crises. They are closely aligned to the Crisis Teams and local acute inpatient units. Some are run by community organisations with service users as key providers.
The houses are located in ordinary streets and normally provide for fewer than 8 people. People usually stay for under three weeks. They are staffed 24hrs a day. Some providers of crisis houses run other crisis services such as family crisis homes. They are fully integrated with home-based treatment, crisis assessment and a day service for people in crisis.
Crisis houses tend to adhere to the view that mental health crises are a turning point and an opportunity for growth rather than just risks that need to be managed. They provide a listening ear, personal support, practical advice and complementary treatments as well as medication. Crisis houses may vary to a degree in their culture and values. Some are very psychosocially-oriented while others use a more equal blend of medical and psychosocial therapies.
Community Housing Support Team (Cornwall)
These are specialised teams consisting of mental health workers, housing experts and community development workers. They are an integral part of the community mental health teams.
The team builds long lasting partnerships with the Housing Sector.
They provide a high level support service to people with a housing need who have difficulty in finding and keeping their accommodation. They work with people who are homeless, threatened with eviction or in unsuitable or insecure housing.
They help people to work towards developing or regaining their skills for independent living by creating an individual housing support plan. Providing information and support for landlords.
Operational Policies will need to be produced for each of the above services
- Steering Committee
A Gwent Steering Committee will be formed consisting of the relevant stakeholders across Gwent. This will oversee the development of the Whole Life-Whole System Model, monitor progress and review the Model in the light of progress with its implementation.
9. Financial Implications
A detailed costing of each component needs to be done.
A BIG Lottery funding application is being prepared for a Crisis House
10. Training Strategy and Program
The development of the Whole Life-Whole System Service Model will also require a change in Thinking and Practice.
Therefore a Training Strategy and Program will need to be established,
- To put the values and principles into practice,
- To change culture, with a change in Thinking and Practice
- To understand and implement the components of the Whole System Service Model
- To introduce new ways of working in the Recovery and Discovery Approach
- Increased psychological therapies and alternative / complementary therapies
John Jenkins
29/09/2016
